What is Psoriasis: Causes, Symptoms, and Treatment
Key Takeaways
- Psoriasis is a chronic autoimmune condition that causes rapid skin cell turnover, leading to red, scaly patches and discomfort.
- Common triggers include stress, infections, skin trauma, certain medications, and lifestyle factors like smoking or alcohol use.
- Treatment may include topical medications, light therapy, systemic drugs, and holistic strategies like anti-inflammatory diets and stress reduction.
- A personalized care plan that includes skincare, nutrition, exercise, and mental health support can significantly reduce symptoms and flare-ups.
Psoriasis is a chronic, non-contagious skin condition that affects millions of people worldwide. Characterized by rapid skin cell production leading to thick, red, scaly patches, psoriasis can cause significant discomfort and impact on quality of life. This blog post delves into what psoriasis is, explores its various types, pinpoints its causes and triggers, and discusses symptoms along with both medical and holistic treatment options. Designed for individuals seeking a deeper understanding of this condition, the content provides valuable insights into managing psoriasis effectively.
What is Psoriasis?
Psoriasis is a complex, chronic autoimmune condition that primarily affects the skin but can also involve other organs and lead to systemic symptoms. It is marked by an overactive immune response that accelerates the lifecycle of skin cells, causing them to multiply at an abnormally fast rate. This rapid turnover results in the buildup of cells on the surface of the skin, forming the characteristic scaly patches known as plaques, which can be painful and itchy.
Types of Psoriasis
Understanding the various forms of psoriasis is essential for effective treatment and management:
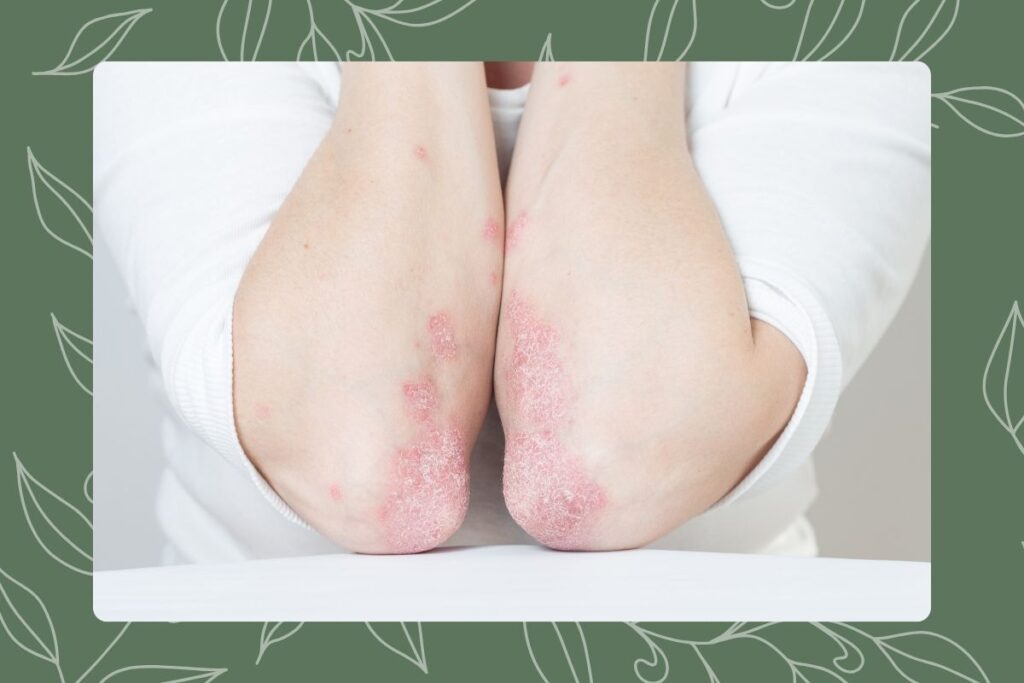
- Plaque Psoriasis: The most prevalent type, affecting about 80% to 90% of psoriasis patients. It features raised, inflamed, red lesions covered by silvery-white scales. Typically found on the elbows, knees, scalp, and lower back.
- Guttate Psoriasis: This form often starts in childhood or young adulthood, presenting as small, water-drop-shaped, scaling lesions on the trunk, arms, legs, and scalp.
- Inverse Psoriasis: Inverse psoriasis manifests as bright red, smooth, and shiny lesions that appear in body folds.
- Pustular Psoriasis: This is a rarer type of psoriasis that causes widespread patches or localized, pus-filled lesions.
- Erythrodermic Psoriasis: The least common type of psoriasis and is a severe form that extensively affects the body surface area.
What Causes Psoriasis?
While the exact cause of psoriasis remains unclear, it is widely acknowledged that a combination of genetic predispositions and environmental factors plays a crucial role. Those with a family history of psoriasis are generally at a higher risk of developing the condition themselves. This susceptibility is due to inherited factors that influence the immune system’s functioning, particularly in how it reacts and leads to the inflammation characteristic of psoriasis.
What Triggers Psoriasis?
Identifying personal triggers is a critical component of managing psoriasis:
- Infections and Illness: Certain infections, particularly bacterial and viral ones, can prompt the onset or aggravation of psoriasis.
- Skin Trauma: Injuries to the skin such as cuts, bruises, or severe sunburns can lead to a flare-up of psoriasis symptoms in a phenomenon known as the Koebner response.
- Lifestyle Factors: Lifestyle choices such as alcohol consumption and smoking have been linked to both the development and exacerbation of psoriasis symptoms.
- Medications: Certain medications, including beta blockers and lithium, have been found to trigger or worsen psoriasis in some people.
- Psychological Stress: Stress is a well-known trigger for psoriasis flares.
Symptoms of Psoriasis
The symptoms of psoriasis are varied and can range from mild to severe:
- Skin Symptoms: Plaques of red skin, often covered with loose, silver-colored scales; these plaques may be itchy and painful and sometimes crack and bleed.
- Scalp Psoriasis: Severe dandruff on the scalp can occur, which is actually psoriatic scales.
- Psoriatic Arthritis: In some cases, psoriasis can lead to psoriatic arthritis. Symptoms include joint pain, stiffness, and swelling.
Psoriasis Treatment Types
Effective treatment for psoriasis often requires a combination of approaches:
- Topical Treatments: Corticosteroids, Vitamin D analogues, and Retinoids are common topical treatments.
- Systemic Treatments: Oral medications like methotrexate and cyclosporine, and biologics targeting specific immune system components.
- Light Therapy: Phototherapy involves regular sessions under medical supervision involving ultraviolet light.
How to Manage Psoriasis Holistically
Adopting a holistic approach can be incredibly beneficial for managing psoriasis. A comprehensive management plan can enhance the body’s ability to cope with this condition, potentially reducing the frequency and severity of flare-ups.
Nutritional Approach
A thoughtful and strategic approach to nutrition can play a pivotal role in managing psoriasis. An anti-inflammatory diet rich in omega-3 fatty acids, antioxidants, and fiber can help control inflammation and support skin health. Foods such as fatty fish (salmon, mackerel), nuts, seeds, and leafy greens are recommended. Additionally, some individuals with psoriasis may benefit from a gluten-free diet, especially if they have a sensitivity to gluten which might exacerbate symptoms.
Physical Activity
Regular exercise is a powerful tool for overall health and can specifically benefit those managing psoriasis. Physical activity helps reduce inflammation, manages weight (obesity can exacerbate psoriasis), and increases the production of endorphins, which are natural mood lifters and pain relievers. Activities like walking, swimming, and cycling are especially beneficial as they are low-impact but help in maintaining an active lifestyle.
Psychological Wellbeing
Managing psychological health is crucial in holistic psoriasis treatment. Stress is a known trigger for psoriasis flare-ups, making stress reduction techniques essential. Practices such as meditation, yoga, and guided relaxation not only help reduce stress but also improve the overall quality of life. Regular participation in these activities can lead to better mental health and potentially fewer psoriasis symptoms.
Alternative Therapies
Alternative therapies such as acupuncture and massage therapy can also support the management of psoriasis. Acupuncture can alleviate stress and pain, while massage therapy reduces stress and improves circulation, which may help decrease the severity and frequency of flare-ups. These therapies should complement traditional treatments as part of a comprehensive approach to managing psoriasis.
Skincare Routine
Maintaining a diligent skincare routine is vital for those with psoriasis. Moisturizing regularly, particularly after bathing, can prevent the skin from drying out, which reduces redness, itching, and the formation of scaly patches. Using fragrance-free and alcohol-free moisturizers is important, as these formulations are less likely to irritate sensitive skin. Additionally, baths with colloidal oatmeal or Epsom salts can soothe and help maintain skin hydration.
Conclusion
Understanding psoriasis from a comprehensive perspective empowers individuals to manage their symptoms effectively and maintain a higher quality of life. Whether through medical treatments or holistic approaches, managing psoriasis requires a personalized strategy that considers various lifestyle factors and potential triggers.
FAQs
What are the main triggers that cause psoriasis to flare up?
Psoriasis triggers vary but commonly include:
- Stress: High stress can lead to flare-ups.
- Skin Injury: Trauma such as cuts, scrapes, or sunburns can trigger psoriasis.
- Infections: Especially streptococcal infections can exacerbate symptoms.
- Weather: Cold and dry conditions may worsen psoriasis; warm, sunny weather might improve it.
- Medications: Certain drugs like beta-blockers and lithium can trigger or worsen symptoms.
Can psoriasis be cured?
There is no cure for psoriasis, but it can be effectively managed with treatments such as topical agents, phototherapy, systemic medications, and biologics. Lifestyle adjustments like diet changes and stress management also play a crucial role in controlling flare-ups.
Is psoriasis contagious?
No, psoriasis is not contagious. It is an autoimmune disorder and cannot be transmitted through skin contact or other physical interactions.
